Everybody loves a bright white smile, and there are a variety of products and procedures available to help you improve the look of yours.
Many people are satisfied with the sparkle they get from brushing twice daily with a fluoride-containing toothpaste, cleaning between their teeth once a day and the regular cleanings at your dentist’s office. If you decide you would like to go beyond this to make your smile look brighter, you should investigate all of your options.
You can take several approaches to whiten your smile:
- At-home bleaching
- Whitening toothpastes
What are at-home procedures and products?
There are several types of products available for use at home, which can either be dispensed by your dentist or purchased over-the-counter.
Bleaching solutions. These products contain peroxide(s), which actually bleach the tooth enamel. These products typically rely on percent carbamide peroxide as the bleaching agent, carbamide peroxide comes in several different concentrations (10%, 16%, 22% and 32%).
Peroxide-containing whiteners typically come in a gel and are placed in a mouthguard. Usage regimens vary. Some products are used twice a day for 2 weeks, and others are intended for overnight use for 1-2 weeks. If you obtain the bleaching solution from your dentist, she can make a custom-fitted mouthguard for you that will fit your teeth precisely.
You also may want to speak with your dentist should any side effects become bothersome. For example, teeth can become sensitive during the period when you are using the bleaching solution. In many cases, this sensitivity is temporary and should lessen once the treatment is finished. Some people also experience soft tissue irritation—either from a tray that doesn’t fit properly or from solution that may come in contact with the tissues. If you have concerns about such side effects, you should discuss them with your dentist.
Toothpastes. All toothpastes help remove surface stain through the action of mild abrasives. “Whitening” toothpastes in the ADA Seal of Acceptance program have special chemical or polishing agents that provide additional stain removal effectiveness. Unlike bleaches, these ADA Accepted products do not alter the intrinsic color of teeth. Before doing these, you should ask an expert who has undergone dental assistant training to know which are effective for your teeth.

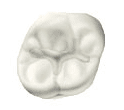 Composite fillings are a mixture of glass or quartz filler in a resin medium that produces a tooth-colored filling. They are sometimes referred to as composites or filled resins. Composite fillings provide good durability and resistance to fracture in small-to-mid size restorations that need to withstand moderate chewing pressure. Less tooth structure is removed when the dentist prepares the tooth, and this may result in a smaller filling than that of an amalgam. Composites can also be “bonded” or adhesively held in a cavity, often allowing the dentist to make a more conservative repair to the tooth.
Composite fillings are a mixture of glass or quartz filler in a resin medium that produces a tooth-colored filling. They are sometimes referred to as composites or filled resins. Composite fillings provide good durability and resistance to fracture in small-to-mid size restorations that need to withstand moderate chewing pressure. Less tooth structure is removed when the dentist prepares the tooth, and this may result in a smaller filling than that of an amalgam. Composites can also be “bonded” or adhesively held in a cavity, often allowing the dentist to make a more conservative repair to the tooth.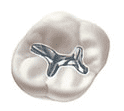 Used by dentists for more than a century, dental amalgam is the most thoroughly researched and tested restorative material among all those in use. It is durable, easy to use, highly resistant to wear and relatively inexpensive in comparison to other materials. For those reasons, it remains a valued treatment option for dentists and their patients.
Used by dentists for more than a century, dental amalgam is the most thoroughly researched and tested restorative material among all those in use. It is durable, easy to use, highly resistant to wear and relatively inexpensive in comparison to other materials. For those reasons, it remains a valued treatment option for dentists and their patients. Gold alloys contain gold, copper and other metals that result in a strong, effective filling, crown or a bridge. They are primarily used for inlays, onlays, crowns and fixed bridges. They are highly resistant to corrosion and tarnishing.
Gold alloys contain gold, copper and other metals that result in a strong, effective filling, crown or a bridge. They are primarily used for inlays, onlays, crowns and fixed bridges. They are highly resistant to corrosion and tarnishing. Another type of restoration is porcelain-fused-to-metal, which provides strength to a crown or bridge. These restorations are very strong and durable.
Another type of restoration is porcelain-fused-to-metal, which provides strength to a crown or bridge. These restorations are very strong and durable.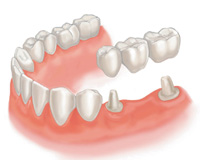 If you’re missing one or more teeth, you may notice a difference in chewing and speaking. There are options to help restore your smile.
If you’re missing one or more teeth, you may notice a difference in chewing and speaking. There are options to help restore your smile.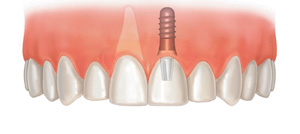 Crowns and conventional bridges or dentures may not be your only options when replacing missing teeth. For some people, dental implants offer a smile that looks and feels very natural. Surgically placed below the gums over a series of appointments, implants fuse to the jawbone and serve as a base for individual replacement teeth, bridges or a denture. Implants offer stability because they fuse to your bone.
Crowns and conventional bridges or dentures may not be your only options when replacing missing teeth. For some people, dental implants offer a smile that looks and feels very natural. Surgically placed below the gums over a series of appointments, implants fuse to the jawbone and serve as a base for individual replacement teeth, bridges or a denture. Implants offer stability because they fuse to your bone.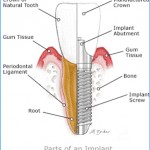
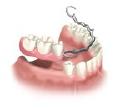 Removable partial dentures usually consist of replacement teeth attached to pink or gum-colored plastic bases, which are connected by metal framework.
Removable partial dentures usually consist of replacement teeth attached to pink or gum-colored plastic bases, which are connected by metal framework.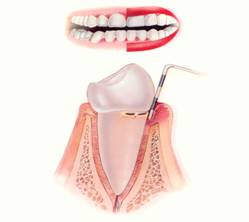 Periodontal disease is an infection of the tissues that support your teeth. Your gum tissue is not attached to the teeth as high as it may seem. There is a very shallow v-shaped crevice called a sulcus between the tooth and gums. Periodontal diseases attack just below the gum line in the sulcus, where they cause the attachment of the tooth and its supporting tissues to break down. As the tissues are damaged, the sulcus develops into a pocket: generally, the more severe the disease, the greater the depth of the pocket.
Periodontal disease is an infection of the tissues that support your teeth. Your gum tissue is not attached to the teeth as high as it may seem. There is a very shallow v-shaped crevice called a sulcus between the tooth and gums. Periodontal diseases attack just below the gum line in the sulcus, where they cause the attachment of the tooth and its supporting tissues to break down. As the tissues are damaged, the sulcus develops into a pocket: generally, the more severe the disease, the greater the depth of the pocket.